TCC-SUP
Cat.No.: CSC-C0425
Species: Homo sapiens (Human)
Source: Bladder
Morphology: epithelial-like adherent cells with smooth borders growing as monolayer
Culture Properties: monolayer
- Specification
- Background
- Scientific Data
- Q & A
- Customer Review
Immunology: cytokeratin -, cytokeratin-7 -, cytokeratin-8 -, cytokeratin-17 -, cytokeratin-18 -, cytokeratin-19
TCC-SUP Cells are human urinary bladder carcinoma cells isolated from a patient with high grade transitional cell carcinoma (urothelial carcinoma). These cells are commonly utilized in research as a cell model to study molecular processes involved in bladder cancer progression, invasion, and therapeutic response in vitro.
Upon cultivation, TCC-SUP cells demonstrate an adherent growth pattern and epithelial-like morphology. Cells often appear polygonal in shape and will grow to confluence as an irregular monolayer. TCC-SUP cells typically express known urothelial and epithelial markers, such as cytokeratins (CK7, CK8, CK18), epithelial cell adhesion molecule (EpCAM), and uroplakin related proteins. TCC-SUP Cells have been found to harbor genetic mutations commonly found in bladder cancer, such as alterations in genes involved in cell cycle regulation, apoptosis, and DNA damage repair.
TCC-SUP Cells have been utilized in assays to study tumor cell proliferation, migration, invasion, and epithelial-mesenchymal transition (EMT). These cells have been used to study signaling pathways commonly dysregulated in bladder cancer including PI3K/AKT signaling, MAPK, and NF-κB. Other studies have utilized these cells to study mechanisms of chemoresistance and tumor aggressiveness. Additionally, these cells have been used for drug screening purposes, cytotoxicity assays, and as models for targeted therapeutics.
AR could Affect PD-L1 Expression in BCa Cells
Androgen receptor (AR) influences bladder cancer (BCa) initiation and progression, but its role in tumor immune escape remains unclear. While AR promotes BCa invasion and cisplatin resistance, whether it affects antitumor immunity by modulating immune cell killing is unknown. Liu's team focused on PD-L1, a critical immune checkpoint molecule and immunotherapy target.
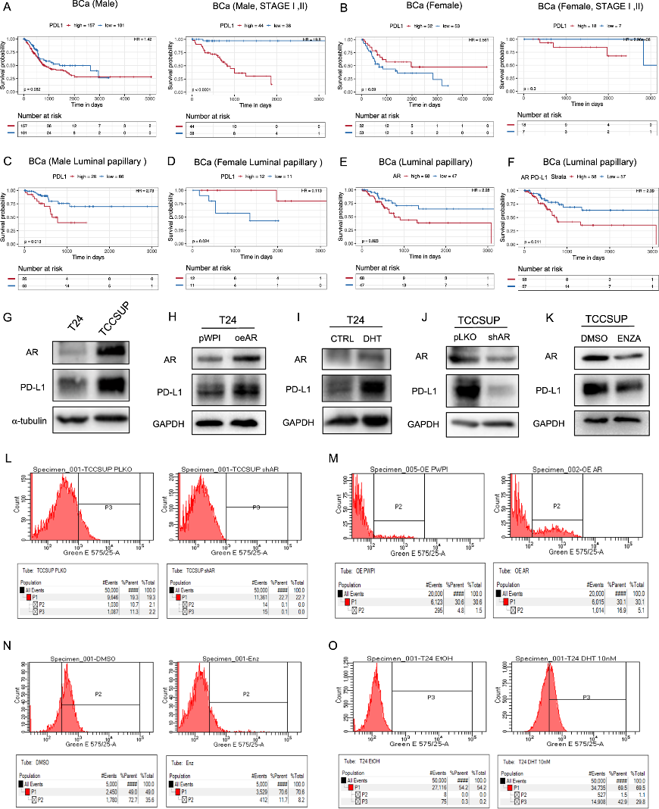
TCGA data showed high AR signaling in the luminal papillary subtype, which is more common in male patients. Analysis of the TRGAted database revealed sex-specific prognostic differences for PD-L1: higher PD-L1 correlated with worse survival in males, particularly in early-stage (I-II) and non-metastatic disease, whereas females showed the opposite trend (Fig. 1A, B). In the luminal papillary subtype, elevated PD-L1 was significantly associated with poor survival in males but not females (Fig. 1C, D). High AR expression also predicted worse progression-free survival in luminal papillary and luminal infiltrated subtypes (Fig. 1E), with combined high AR/PD-L1 indicating the poorest outcomes (Fig. 1F).
To examine whether AR regulates PD-L1, they used T24 (low AR) and TCC-SUP (high AR) BCa cell lines. AR overexpression and androgen (DHT) treatment upregulated PD-L1 in T24 cells (Fig. 1G-I), while AR knockdown and antiandrogen (Enz) treatment downregulated PD-L1 in TCC-SUP cells (Fig. 1K). Additional antiandrogens (HF) and the AR degrader ASC-J9 similarly reduced PD-L1. Flow cytometry confirmed that membrane PD-L1 levels paralleled AR activity: DHT increased and Enz decreased surface PD-L1 expression (Fig. 1L-O). These data demonstrate that AR signaling regulates PD-L1 expression in BCa cells.
Ask a Question
Write your own review
- You May Also Need
- Adipose Tissue-Derived Stem Cells
- Human Neurons
- Mouse Probe
- Whole Chromosome Painting Probes
- Hepatic Cells
- Renal Cells
- In Vitro ADME Kits
- Tissue Microarray
- Tissue Blocks
- Tissue Sections
- FFPE Cell Pellet
- Probe
- Centromere Probes
- Telomere Probes
- Satellite Enumeration Probes
- Subtelomere Specific Probes
- Bacterial Probes
- ISH/FISH Probes
- Exosome Isolation Kit
- Human Adult Stem Cells
- Mouse Stem Cells
- iPSCs
- Mouse Embryonic Stem Cells
- iPSC Differentiation Kits
- Mesenchymal Stem Cells
- Immortalized Human Cells
- Immortalized Murine Cells
- Cell Immortalization Kit
- Adipose Cells
- Cardiac Cells
- Dermal Cells
- Epidermal Cells
- Peripheral Blood Mononuclear Cells
- Umbilical Cord Cells
- Monkey Primary Cells
- Mouse Primary Cells
- Breast Tumor Cells
- Colorectal Tumor Cells
- Esophageal Tumor Cells
- Lung Tumor Cells
- Leukemia/Lymphoma/Myeloma Cells
- Ovarian Tumor Cells
- Pancreatic Tumor Cells
- Mouse Tumor Cells