Chronic Liver Injury Models
Chronic liver injury manifests in various chronic liver disease forms, including chronic hepatitis, liver cirrhosis, chronic intrahepatic cholestasis, sclerosing cholangitis, fatty liver, heparin accumulation syndrome, sinusoidal obstruction syndrome/hepatic venous occlusive disease, liver tumors, idiopathic portal hypertension, etc. Faced with such a wide variety of liver diseases, researchers need pre-clinical models to ensure the safety and effectiveness of new drugs or therapies.
With years of professional experience in chronic liver disease, Creative Bioarray provides a variety of customized in vivo chronic liver disease models to solve critical problems for customers.
Chronic liver injury models
- Carbon tetrachloride (CCl4)
CCl4 is a widely used chemical for experimental induction of fatty liver, liver cirrhosis, and liver fibrosis in animals. CCl4 causes acute liver damage in mice mainly by destroying the liver cells of the mice. Alanine aminotransferase (ALT) and aspartate aminotransferase (AST) in the liver cells enter the blood through the liver cell membrane, leading to increased transaminase activity in the blood. Carbon tetrachloride can also produce high-energy reactions through the biotransformation of the cytochrome P450 system, thereby inducing liver damage.
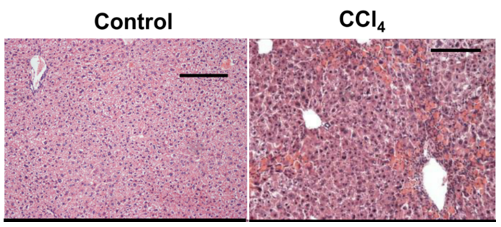 Figure 1. Hematoxylin and eosin staining chronic liver injury induced by CCl4 (Brol et al., 2019).
Figure 1. Hematoxylin and eosin staining chronic liver injury induced by CCl4 (Brol et al., 2019).
- Bile duct ligation (BDL) induced liver fibrosis
The surgical method of liver fibrosis is to expose and ligate the bile ducts by surgery, directly causing cholestasis, a model of cholestatic liver fibrosis characterized by bile duct hyperplasia. Bile duct ligation can be used to ligate the common bile duct in animals by surgery or using inhibitors on cells in vitro to cause bile obstructive lesions. To a certain extent, bile duct ligation can better simulate the process of human hepatocyte proliferation and apoptosis, portal fibrosis, and liver cirrhosis caused by long-term cholestasis, as well as the common complications of biliary acute kidney injury.
- Combined factor-induced liver cirrhosis and fibrosis
The factors that lead to liver disease are complex and changeable, and even a variety of compound factors affect the formation and development of liver disease. In particular, liver fibrosis is the central link in the development of liver disease. Therefore, establishing an animal model of liver fibrosis with compound injury is of great clinical necessity and meets liver disease epidemiology. The establishment of a composite liver fibrosis model adopts compound factors such as ethanol gavage, high-fat feed feeding, high-sugar drinking water, etc., combined with an improved version of the combined method of intraperitoneal injection of CCl4.
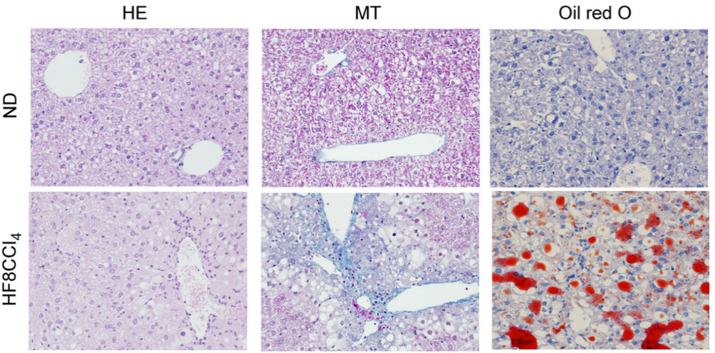 Figure 2. Liver histology in mice fed the normal diet (ND), high-fat diet alone (HF), and the high-fat diet plus CCl4 (administered s.c. twice a week for the final 4 weeks of feeding; HF8CCl4). HE, hematoxylin, and eosin staining; MT, Masson's trichrome staining(Kubota et al., 2013).
Figure 2. Liver histology in mice fed the normal diet (ND), high-fat diet alone (HF), and the high-fat diet plus CCl4 (administered s.c. twice a week for the final 4 weeks of feeding; HF8CCl4). HE, hematoxylin, and eosin staining; MT, Masson's trichrome staining(Kubota et al., 2013).
- ALD/ ASH
Alcoholic liver disease (ALD), which includes alcoholic steatohepatitis (ASH), refers to the accumulation of fat in liver cells due to alcohol damage, the formation of fibrosis, and the gradual development of liver cirrhosis. Using the known clinical symptoms of liver disease, modeling in animals with similar mechanisms to humans, and studying its pathogenesis and causes are significant for classifying and treating modern liver diseases.
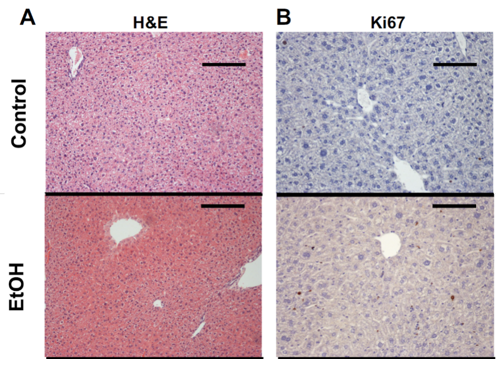 Figure 3. Proliferation assessment of the animal models. Hematoxylin and eosin (H&E, A), Ki-67 immunohistochemistry staining (B) with its quantification(Brol et al., 2019).
Figure 3. Proliferation assessment of the animal models. Hematoxylin and eosin (H&E, A), Ki-67 immunohistochemistry staining (B) with its quantification(Brol et al., 2019).
- NAFLD/ NASH
Non-alcoholic liver disease (NAFLD), which includes non-alcoholic steatohepatitis (NASH), refers to the damage of liver cells formed by eliminating alcohol and other definite causes of liver damage. Its pathological feature is the accumulation of a large amount of fat in the liver, leading to the excessive proliferation of muscle fibers and aggravating liver fibrosis formation. The use of a high-fat diet can induce liver fibrosis in rats within 8 weeks. Moreover, the above-mentioned "Combined factor-induced liver cirrhosis and fibrosis" is also a strategy for constructing NAFLD models. Also, We can also use gene-edited animals to construct NAFLD/NASH animal models, such as ob/ob and db/db mice.
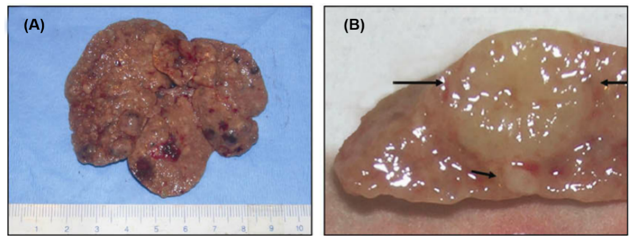 Figure 4. Liver phenotype. (A) Steatotic and cirrhotic appearing liver. (B) Large focal lesion with small lesion inferiorly(de Lima et al., 2008).
Figure 4. Liver phenotype. (A) Steatotic and cirrhotic appearing liver. (B) Large focal lesion with small lesion inferiorly(de Lima et al., 2008).
Species
- Mice
- Rats
- Non-human primates (NHP)
Available Assays
- Cytotoxicity assays
- Measurement of cytokines
- Flow cytometric analysis of cell death
- Measurement of serum liver enzymes
- Hematoxylin and eosin staining (H&E)
- Immunohistochemistry
- Quantitative real-time PCR
- TUNEL stain
- Western blot analysis
- Gene expression analysis
- Oil red O staining
- Masson's trichrome staining
Applications
- To help study the etiology and pathological characteristics of diseases and propose new etiological hypotheses and treatment methods.
- To explore the mechanism of drug action.
- To verify the function of new genes
- To better study the pathogenesis of liver fibrosis and seek better drugs to reverse the process of fibrosis.
Quotation and ordering
If you have any special needs or questions regarding our services, please feel free to contact us. We look forward to cooperating with you in the future.
References
- Brol, M. J.; et al. Combination of CCl4 with alcoholic and metabolic injuries mimics human liver fibrosis. American Journal of Physiology-Gastrointestinal and Liver Physiology, (2019), 317(2), G182-G194.
- de Lima, V. M. R.; et al. A rodent model of NASH with cirrhosis, oval cell proliferation and hepatocellular carcinoma. Journal of Hepatology, (2008), 49(6), 1055-1061.
- Kubota, N.; et al. A high-fat diet and multiple administration of carbon tetrachloride induces liver injury and pathological features associated with non-alcoholic steatohepatitis in mice. Clinical and Experimental Pharmacology & Physiology, (2013), 40(7), 422-430.