Human Renal Mesangial Cells (HRMC)
Cat.No.: CSC-7719W
Species: Human
Source: Kidney
Cell Type: Mesangial Cell
- Specification
- Background
- Scientific Data
- Q & A
- Customer Review
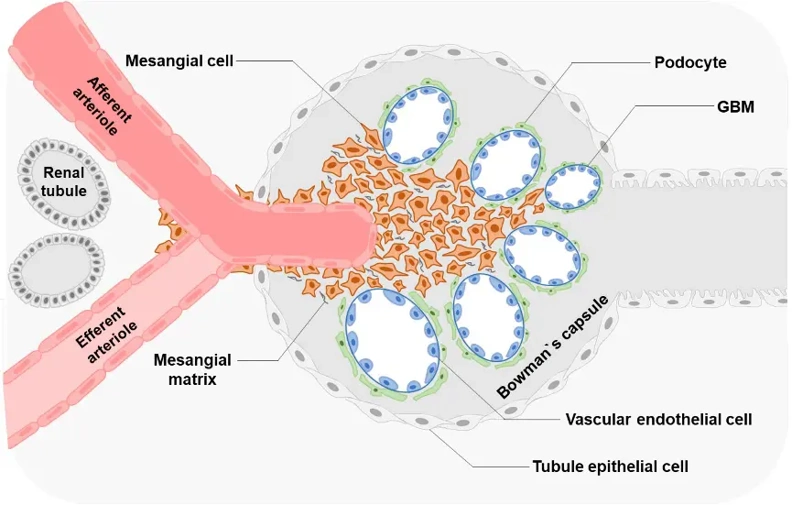
Human Renal Mesangial Cells (HRMC) are primary cells derived from the glomerular mesangium of human kidneys. These cells provide an important physiologically relevant in vitro model to study glomerular function and to further understand the mechanisms underlying renal disease. Mesangial cells are specialized pericytes located within the glomerulus that are responsible for providing mechanical support to the capillary loops, regulating glomerular capillary blood flow, and turnover of extracellular matrix within the glomerulus.
HRMCs are stellate or spindle shaped under standard culture conditions and are grown as adherent monolayers. They have been shown to express mesangial cell markers such as α-smooth muscle actin (α-SMA), desmin, and platelet-derived growth factor receptor-β (PDGFR-β) to demonstrate their mesenchymal like phenotype. HRMCs have been shown to contract in response to vasoactive factors and growth factors and release inflammatory mediators in response to inflammatory stimuli. Specifically, they respond to angiotensin II, platelet-derived growth factor, and transforming growth factor-β (TGF-β).
HRMCs have been used to study the pathogenesis of several glomerular diseases such as diabetic nephropathy, glomerulonephritis, and renal fibrosis. These cells have also been used as an in vitro model to study mesangial cell proliferation, mesangial matrix expansion, oxidative stress, and inflammatory pathways associated with progressive renal injury. HRMCs can also be used to screen potential renoprotective and anti-fibrotic therapies.
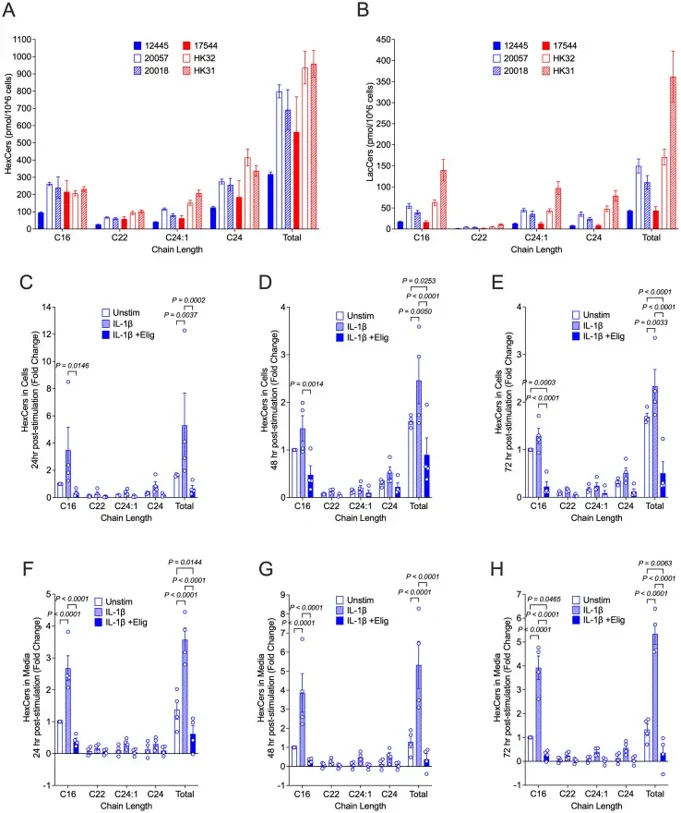
IL-1β Treatment Significantly Increases Cellular and Excreted Levels of HexCers that are Reduced by Treatment with Eliglustat
Glycosphingolipids (GSLs)-including hexosylceramides (HexCers), lactosylceramides (LacCers), and gangliosides-are essential membrane components whose dysregulated metabolism has been implicated in inflammatory diseases such as lupus nephritis, though their role in renal cell dysfunction remains unclear.
Primary human renal mesangial cells (hRMCs) were treated with proinflammatory cytokines (IL-1β, TNFα, IFNγ, IFNα) ± eliglustat (an FDA-approved GSL synthesis inhibitor), with HexCer levels, viability, and cytokine secretion assessed by HPLC-MS/MS, alamar blue, and ELISA. Given the prior observation of sex-dependent inflammatory responses in fetal hRMCs, Stefanenko et al. compared GSL levels across fetal and adult cells (2 male, 2 female; all passage 6, ~90% confluence, analyzed simultaneously). Basal GSL levels varied across individuals (Fig. 1A, B), with greater variability in LacCers than HexCers. ince HexCers (GalCers + GlcCers) are the initial GSLs generated from ceramide, they assessed their response to stimulation. IL-1β significantly increased cellular HexCers at 24h, 48h, and 72h (Fig. 1C-E), with similar fold changes across all cell lots. Excreted HexCers also increased significantly (Fig. 1F-H), suggesting IL-1β induces GSL synthesis and that cellular export of excess GSLs may serve to maintain homeostatic levels.
Ask a Question
Write your own review