Human Chorionic Mesenchymal Stromal Cells (HCMSC)
Cat.No.: CSC-7809W
Species: Human
Source: Chorion; Placenta
Cell Type: Stromal Cell
- Specification
- Background
- Scientific Data
- Q & A
- Customer Review
Human Bronchial Epithelial Cells - Asthma are spontaneously growing primary airway epithelial cells that are derived from bronchial tissue obtained from patients with asthma. They maintain many disease-relevant phenotypic characteristics of asthmatic airway epithelium and serve as a clinically relevant in vitro model system for investigating asthma pathogenesis and airway inflammation.
Histologically, human asthma bronchial epithelial cells possess a cobblestone morphology characteristic of epithelial cells and are adherent cells that form monolayers when cultured under normal conditions. Functionally, they have been shown to have disrupted barrier function, disorganized tight junctions, and increased epithelial permeability compared to normal bronchial epithelial cells. They have also been found to have altered expression of cytokines, chemokines and other inflammatory mediator characteristic of chronically inflamed airways such as increased production of IL-6, IL-8 and thymic stromal lymphopoietin (TSLP).
Human Bronchial Epithelial Cells - Asthma have been used as a model to study epithelial-mediated immune reactions, airway remodeling and epithelial-immune cell interactions seen in asthma. They can be stimulated to study reactions to allergens, environmental triggers, and viruses. Human bronchial epithelial cells - asthma are also used to screen for anti-inflammatory and anti-asthmatic drug candidates.
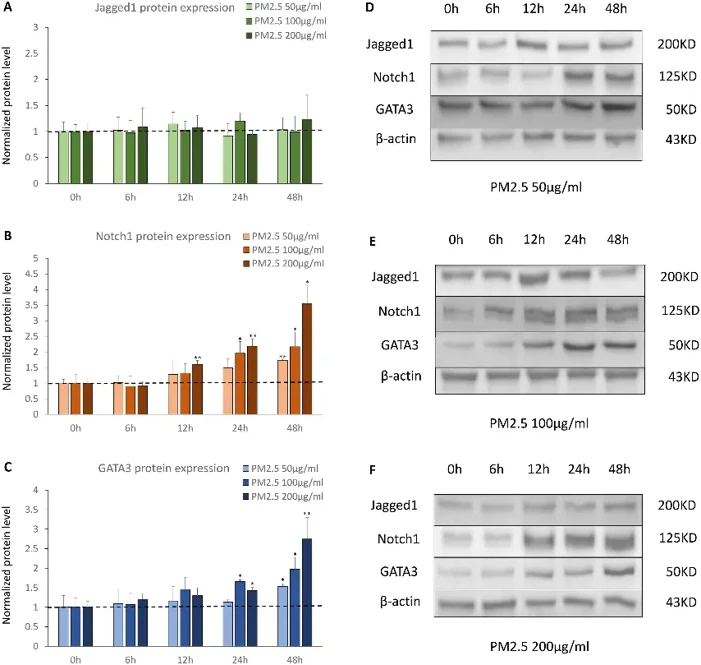
Acute PM2.5 Exposure Activated Notch1-GATA3 Signal Pathway of D-HBE-As Cells
PM2.5 exposure exacerbates asthma through mechanisms involving the Notch1 pathway and Th2 cell differentiation. While miR-139-5p regulates Notch1 in cancer, its role in asthma remains unexplored. Huang's team hypothesized that acute PM2.5 exposure induces asthma exacerbation by modulating miR-139-5p and activating the Notch1-GATA3 pathway.
Using Diseased Human Bronchial Epithelial Cells-Asthma (D-HBE-As), they established an acute PM2.5 exposure model with low (50 µg/ml), middle (100 µg/ml), and high (200 µg/ml) doses for 0-48 h. Jagged1 expression remained unchanged across all conditions (Fig. 1A). However, Notch1 protein increased from 12 h onwards in a dose- and time-dependent manner, with earlier and more pronounced elevation at higher concentrations (Fig. 1B). GATA3 followed a similar pattern but with delayed onset at 24 h (Fig. 1C), suggesting PM2.5 sequentially activates Notch1-GATA3 signaling in asthmatic bronchial epithelium.
Ask a Question
Write your own review