Primary Bovine Aortic Endothelial Cells
Cat.No.: CSC-C4393X
Species: Bovine
Source: Aorta
Cell Type: Endothelial Cell
- Specification
- Background
- Scientific Data
- Q & A
- Customer Review
Primary Bovine Aortic Endothelial Cells (BAECs) are endothelial cells derived from the luminal surface of the aorta and provide a widely used in vitro model system for vascular biology and cardiovascular research. As primary cells derived directly from tissue, BAECs preserve many of the important physiological and phenotypic features of endothelial cells in vivo, including displaying a typical "cobblestone" appearance when confluent. In addition, primary BAECs have not been transformed or immortalized and therefore display endothelial cell-relevant biological behaviors such as expressing endothelial cell markers including von Willebrand factor (vWf) and CD31 (PECAM-1). BAECs are able to be easily isolated due to the large surface area of the bovine aorta and demonstrate strong growth profiles allowing for high yield cultures. For these reasons, BAECs are often used to study basic vascular biology such as angiogenesis, vascular permeability and hemodynamic shear stress as well as the mechanisms involved in cardiovascular diseases like atherosclerosis and hypertension.
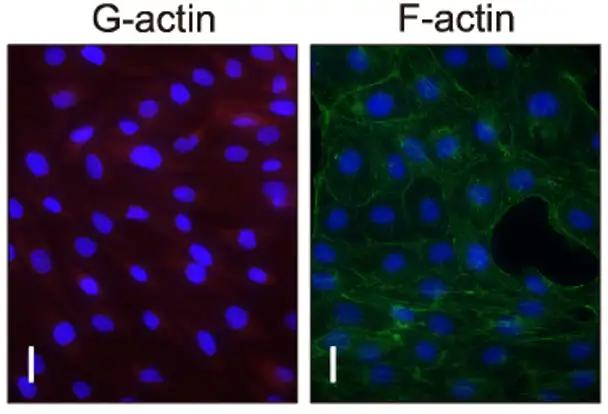
NaCl Impairs Migration and Angiogenic Potential of BAECs In Vitro
High salt intake is associated with hypertension; however, the precise molecular mechanisms underlying salt-mediated endothelial dysfunction leading to increased blood pressure remain unclear. Li et al. explored the impact of high salt consumption on endothelial dysfunction and hypertension, specifically examining the role of O-GlcNAc modification of endothelial nitric oxide synthase (eNOS).
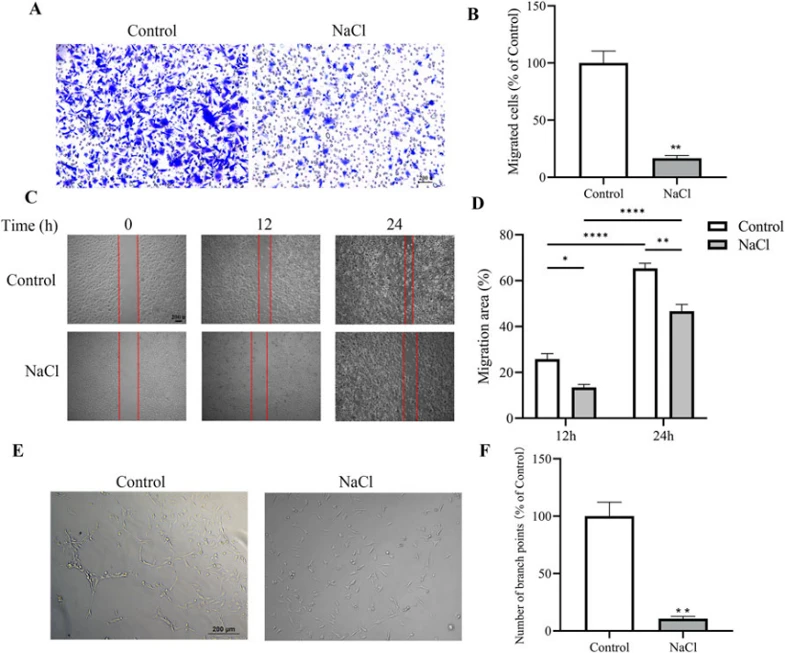
Endothelial cells play a pivotal role in maintaining vascular homeostasis. To examine the direct impact of high salt on endothelial cells, Li's group treated BAECs with NaCl in vitro followed by functional assays. In transwell migration assay, NaCl-treated cells exhibited impaired migratory ability, with decreased cell numbers migrating through the membrane pores and less crystal violet staining intensity compared to controls (Fig. 1A, B). Similar results were seen in wound healing assays as NaCl-treated cells displayed delayed scratch closure and significant reduction in migration distance compared to control scratches (Fig. 1C, D). Furthermore, NaCl-treated BAECs had reduced capacity to form capillary-like structures with fewer branch points and malformed structures in tube formation assays (Fig. 1E, F). Taken together, these findings reveal that high concentrations of extracellular NaCl directly inhibits endothelial cell migration and angiogenesis.
Ask a Question
Write your own review